A Voice for Cooper
First a car wreck would save Cooper Kilburn’s life. Two years later, an innovative surgery would change it.
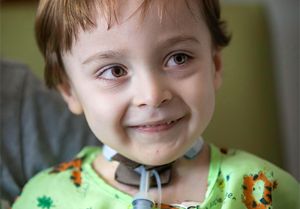
Cooper was born with no airway, no larynx and, therefore, no voice. He relied on a trach to breathe. He slept on a ventilator to survive the nights. And at 2 years old, he had never made a sound. Not a cry. Not even a whimper.
And that’s how this story begins. Lucky for Cooper, his medical team made sure that wasn’t the end.
On February 27, 2019, Cooper became the world’s first recorded child born with no airway or larynx to successfully undergo voice box reconstruction. The surgery, led by Le Bonheur Otolaryngologist Jerome Thompson, MD, used a rib graft to create the voice box and establish a viable airway.
Ten weeks later, he made sounds for the first time – laughing with his mom in the comfort of his home.
“I thought I must be dreaming,” said Cooper’s mom, Brooke. “I called Dr. Thompson to listen over the phone and confirm — we were finally hearing Cooper make his first noises.”
The story of Cooper’s voice, Brooke will tell you, is an unlikely one. Because if it wasn’t for a car wreck at the start of a family vacation, the Kilburns would have lost their son before he was born.
ALL IT TAKES IS FIVE PERCENT
Brooke Kilburn of Adamsville, Tenn., was 16 weeks pregnant with Cooper when she was in a car accident. Shaken but
unhurt, she went to her obstetrician for an ultrasound to make sure all was well with her child.
“The obstetrician saw something wrong but didn’t know what it was,” said Brooke. “A specialist in Jackson, Tenn., told us he had never seen anything like this before. He prepared us for the worst case scenario.”
An ultrasound revealed fluid was building in Cooper’s chest because of a rare condition – total laryngeal agenesis due to congenital high airway obstruction syndrome (CHAOS).
Cooper had no airway and no way to breathe outside the womb.
“The fluid had started to compress Cooper’s heart,” said Brooke. “If we hadn’t had that wreck it would have been too late for him.”
As it was, Cooper had a five percent chance of being born alive.
BEATING THE ODDS
Brooke and Brad Kilburn quickly began searching for ways to save Cooper’s life.
Their first stop was St. Louis Children’s Hospital where a surgeon was able to take enough fluid out of Cooper’s chest in utero to relieve the pressure on his heart. But that was all he was able to do. His recommendation – take Cooper to Memphis and Le Bonheur Children’s.
“Both our specialist in Jackson and surgeon in St. Louis mentioned Le Bonheur’s expertise for Cooper,” said Brooke. “We knew that Le Bonheur specialized in children and that with the help of Dr. Thompson, Le Bonheur was the only place that Cooper could be born.”
In conjunction with Le Bonheur Children’s Hospital’s Fetal Center, Thompson put together a plan for Cooper to survive delivery. Cooper would be delivered at a neighboring birthing hospital and then transported to Le Bonheur’s Neonatal Intensive Care Unit (NICU).
At birth, Thompson immediately performed an ex utero intrapartum treatment (EXIT) procedure, a partial
caesarean section that allowed Cooper to continue to receive oxygen via the placenta.
“Cooper’s lack of airway required that we leave him attached to his mom via the umbilical cord as long as possible,” said Thompson. “The EXIT procedure allowed us to remove the fluid from his lungs and perform a tracheostomy prior to his full delivery.”
After remaining in Le Bonheur’s NICU for 324 days, Cooper had beaten the odds. But it was just the beginning of the road for the Kilburn family. Even at home Cooper remained dependent on a trach at all times and a ventilator at night. If his trach clogged, he would not survive. The Kilburns knew that Cooper’s chances for mortality increased every year that he remained on the trach.
Cooper needed an airway.
A REVOLUTIONARY SURGERY
Two years and eight surgeries later, the Kilburns were back at Le Bonheur. This time they saw light at the end of the tunnel.
“Over the first two years of his life, Cooper had done remarkably well and continued to follow normal development milestones,” said Thompson. “Our goal for surgery was to create an anatomical airway, get him off the trach and, possibly, give him a voice.”
To date, there have only been a handful of documented attempts to create an anatomical airway from scratch – all of which have been unsuccessful. If Cooper’s surgery was a success, he would be the first recorded child born with total laryngeal agenesis to have reconstruction of an airway and a larynx. During Cooper’s previous procedures, Thompson had seen embryological vocal cords and knew Cooper still had a chance to make sounds.

Cooper’s surgery and care was a collaborative effort between various divisions of Le Bonheur, including ENT, neonatology, pulmonology, pediatric surgery and the ICU.
“We planned for this surgery from day one of Cooper’s life,” said Thompson. “Everyone from the nurses to surgery technicians to the neonatal team rose to the challenge and worked together for this surgery to be a success.”
Thompson and his team had confidence that they could create an airway for Cooper because they had done it before – just not to this extent. Previous airway reconstruction patients at Le Bonheur had some sort of laryngeal structures, but Cooper had none. Cooper’s health improvement had plateaued. The time for the surgery was now.
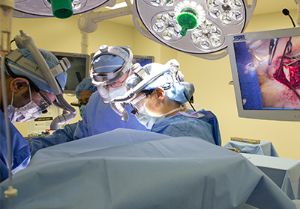
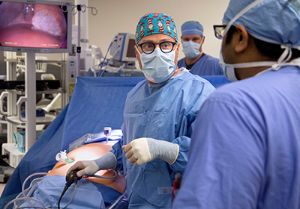
The four-hour surgery was conducted in tandem by Pediatric Surgeon Ying Zhuge, MD, and Thompson. Zhuge removed two of Cooper’s cartilaginous ribs to use to construct the voice box.
Subsequently, Thompson made his first incisions to uncover the abnormalities in Cooper’s laryngeal anatomy — a “conglomerate of embryological mistakes,” according to Thompson. Where there should have been hollowed out spaces, there were round marbles of cartilage. Underdeveloped muscles and cartilage were in all the wrong places.
We planned for this surgery from day one of Cooper's life. Everyone from the nurses to surgery technicians to the neonatal team rose to the challenge and worked together for this surgery to be a success.
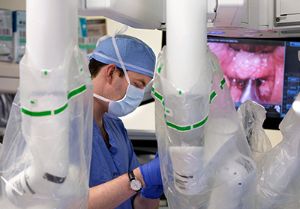
While his thyroid cartilage was normal, his cricoid, a signet-ring shaped piece of cartilage below the thyroid cartilage, was unlike anything Thompson had ever seen. A rock-hard triangular-shaped structure sat where his windpipe should have been. Through this rock-hard cartilage, Thompson and his associate, Otolaryngologist Jennifer McLevy, MD, used needles and a camera to establish a midline for the airway between Cooper’s vocal cords.
Thompson then used the ribs to create the front and back walls of a voice box, thus establishing a new airway. The surgery ended with a stent inserted to hold everything in place while mucous membranes grew around the newly inserted ribs.
The next step was the hardest — waiting six weeks for the stent to be removed to see if Cooper would have an airway.
COOPER'S FUTURE
Six weeks later, Thompson removed the stent to find what he had been hoping for — Cooper now had a new anatomical airway. During the six weeks that the stent was in place, a fibrous envelope had grown around the grafted ribs, allowing the airway to retain its structure when the stent was removed.
At a recent follow-up appointment, a small piece of string determined whether or not Cooper’s airway was viable. The smallest movement of the string as Thompson held it to Cooper’s nose showed that, yes, the surgery had been a success and Cooper was breathing through his new airway.
Cooper’s journey is ongoing. He undergoes a laser treatment every two weeks to remove scar tissue from the new airway and still has surgeries planned for the future to reconstruct his epiglottis so he can eat safely.
He saved our son's life and even gave him a voice we didn’t think he would ever have.
But the benefits of the surgery are already evident. While only the size of a pinky finger, this new airway gives Cooper a better chance at life. Brooke and Brad no longer have to worry about Cooper’s trach plugging. He has a new airway.
And he has even started making sounds for the first time in his life.
“We can’t thank Dr. Thompson and Le Bonheur enough for what they have done for Cooper,” said Brooke. “He saved our son’s life and even gave him a voice we didn’t think he would ever have.”
Help us provide the best care for kids.
Le Bonheur Children's Hospital depends on the generosity of friends like you to help us serve 250,000 children each year, regardless of their family’s ability to pay. Every gift helps us improve the lives of children.
Donate Now