Extracorporeal Membrane Oxygenation (ECMO) is a treatment that uses a heart and a lung machine to support children when their organs are too weak to support the body’s needs. ECMO is not a permanent solution and is used when standard treatments fail. It gives times for the doctors to treat the underlying illness and the body to heal itself.
How does ECMO work?
ECMO uses a pump to take over the work of the heart and an artificial lung to take over the work of the lung. One or two large tubes known as cannulas are inserted in the neck or groin. These act like large IVs that pull blood from the body into the ECMO pump.
Once blood enters the ECMO pump, it pushes the blood into the artificial lung, which removes carbon dioxide and adds oxygen. Then, the treated blood is warmed before re-entering the body.
Types of ECMO treatment
Veno-Arterial ECMO (VA): VA ECMO takes over the function of the heart and the lungs and gives them time to rest. In VA ECMO, one cannula is surgically placed into an artery and one cannula is surgically placed into a vein.
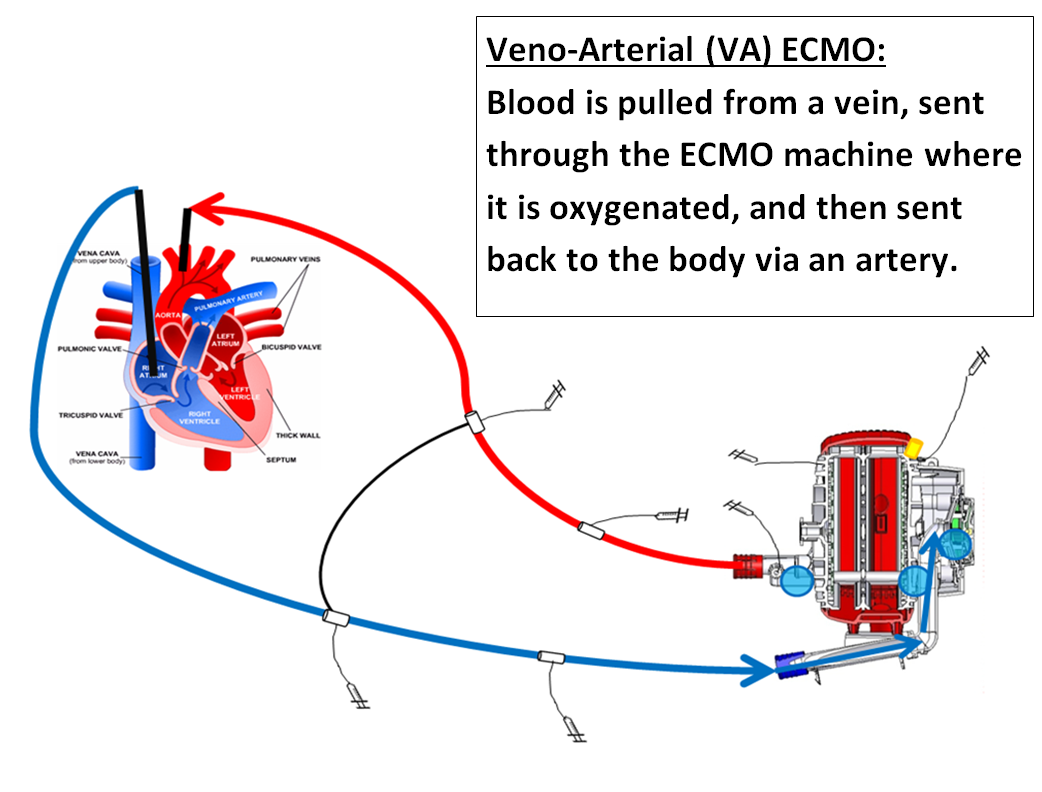
Veno-Venous ECMO (VV): VV ECMO takes over the function of the lungs and gives them time to rest. In VV ECMO, one or two cannulas are surgically placed in one or two veins. In infants, a special cannula that has two very small tubes inside it may be used instead of two cannulas.
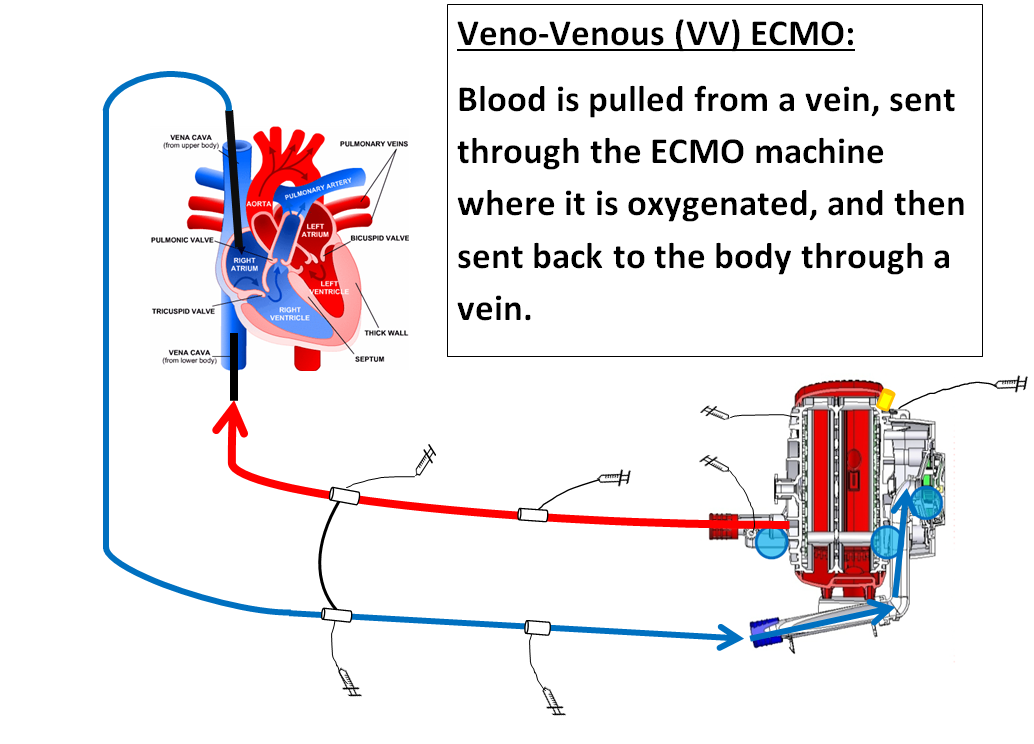
When does a child need ECMO treatment?
- To give rest to the lungs/heart while the initial cause of illness is treated.
- Newborn respiratory failure
- Extra support before or after heart surgery
- As a bridge to a heart or lung transplant while the child awaits a new organ
- Severe Pneumonia or viral flu (influenza)
How long will ECMO be used?
The time a child spends on ECMO depends on the amount of rest and recovery the body needs. The goal is to stop the use of the ECMO machine as soon as the child is ready. The care of the child is discussed in daily rounds at the child's bedside with the doctors and the ECMO medical team.
The Le Bonheur ECMO Team
Le Bonheur has been providing ECMO treatments to neonatal and pediatric patients since 1990. We have been members of Extracorporeal Life Support Organization (ELSO) for the past 25 years. We are the only pediatric ECMO program in the region. The ECMO team consists of doctors, nurses, respiratory therapists, and others who provide the best possible care of the child.
- ECMO Medical Director: Le Bonheur's ECMO medical directors are Hitesh Sandhu, MB, BS, MRCPCH and Samir Shah, MD, MBA. They are the doctors responsible for the medical management and supervision of the ECMO program.
- ECMO Attending Physician: ECMO attending physicians are primary intensive care doctors who have specialized training in the care of critically ill children and infants. They are responsible for the day-to-day medical management of the ECMO patient with the help of the ECMO team.
- Pediatric Surgeons: Your ECMO team includes surgeons specialized in surgical procedures for children. Either a general pediatric surgeon or a pediatric cardiothoracic surgeon will initiate ECMO and will be part of the child’s plan of care while on ECMO
- ECMO Supervisor: Le Bonheur’s ECMO director is Katy Rower, MBA-HM, BSN, RN. She is responsible for the management of the ECMO program.
- ECMO Coordinator: Le Bonheur's ECMO coordinator is Sarah Downing, BSN, RN. She is responsible for the day-to-day management of the ECMO program and training of the ECMO staff.
- ECMO Primers: An ECMO Primer is a senior ECMO specialist who is trained to help the surgeons place a patient on ECMO, assist with troubleshooting, intra-hospital transport, and emergencies.
- ECMO Specialists: ECMO specialists are registered nurses or registered respiratory therapists experienced in pediatric care. They have specialized training in the management and care of the patient and the ECMO machine.



