Bumps and Rashes: Common Skin Conditions Explained
Posted: April 15, 2026It often starts small, like a red patch, a mysterious bump or a rash you didn’t notice the day before. In a blink, it’s itchy, irritated and leads to a visit to your child’s primary care provider.
Sensitive skin, developing immune systems, everyday play and hygiene make kids prone to these issues. The good news is that many childhood skin conditions are harmless and often resolve on their own, but some may deserve a closer look.
Dr. Stephen Bauch, MD, with Le Bonheur Pediatrics, breaks down what’s common and when to seek medical advice so you’re prepared when something unfamiliar pops up.
Viral Rash (Viral Exanthem)
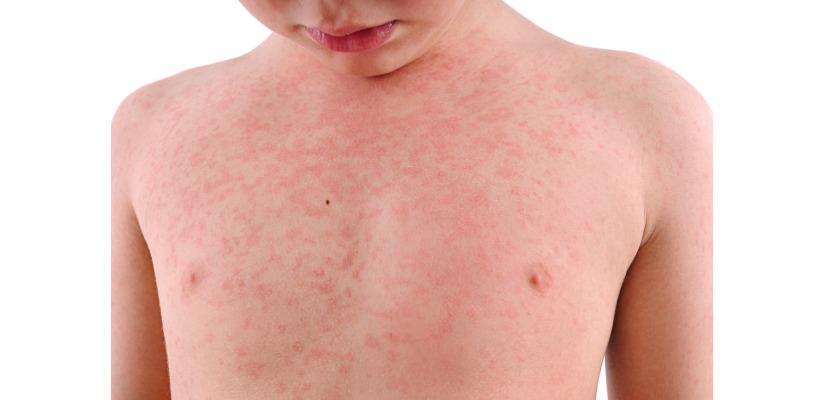
Caused by common viruses like enteroviruses, roseola, adenovirus and others, this rash often occurs during or after a viral illness like a cold or a fever.
It’s usually harmless and goes away on its own. Most viral rashes are benign and part of the body's normal response to fighting infection.
It is contagious, and the underlying virus can spread to others through respiratory droplets or direct contact. Your child is most contagious before and during the early stages of illness.
Does it need treatment?
No specific treatment is needed for the rash itself. Focus on treating symptoms like fever and discomfort. You can give acetaminophen (Tylenol) for fever and discomfort. Keep your child comfortable, well-hydrated and let the rash run its course.
When to see your child’s provider or a specialist?
- If your child has severe pain, trouble breathing, or looks very ill
- If the rash develops blisters around the eyes, mouth or genitals
- If you see signs of infection (yellow/green fluid, warmth, red streaks)
- If your child has a high fever that won't come down or lasts more than a few days
Interesting fact: Viral rashes are sometimes mistaken for drug allergies. About 10% of suspected drug allergies in children are actually just viral rashes that happened to appear while the child was taking medication for a viral infection.
Heat Rash (Pricky Heat or Miliaria)
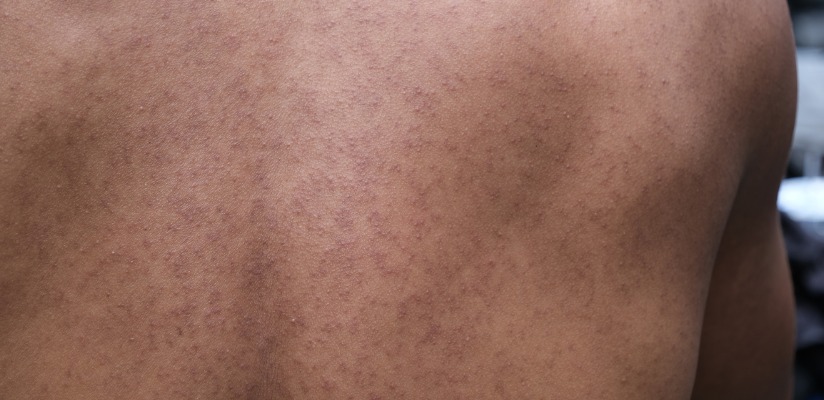
Heat Rash appears when blocked sweat glands trap sweat under the skin. It happens in hot, humid weather or when babies are overdressed or bundled too warmly. It’s harmless and usually clears up on its own once the child cools down. This rash is not contagious.
Does it need treatment?
Usually, no treatment is needed, and cooling measures are typically enough.
To make your child more comfortable, move them to a cooler environment, remove excess clothing or blankets, keep the skin dry and avoid heavy creams or ointments that can block pores and dress your child in loose, lightweight clothing.
When to see your child’s provider or a specialist?
- If the rash doesn't improve with cooling measures
- If you see signs of infection (redness, warmth, pus)
- If your child develops a fever or seems uncomfortable
Interesting fact: Prickly heat is especially common in newborns because their sweat glands aren't fully developed yet. Some babies can even be born with it if the mother had a fever during labor.
Eczema (Atopic Dermatitis)
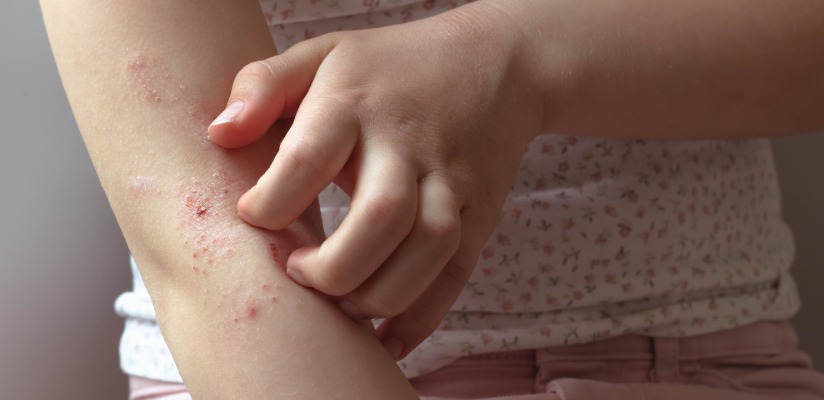
A combination of genetic factors and environmental triggers can lead to eczema. Skin barrier problems, immune system responses and families with a history of eczema, allergies or asthma are most susceptible.
Eczema can be uncomfortable and affect quality of life. Skin infections are possible if you scratch excessively. Eczema is not contagious. It is a chronic condition with flare-ups and calm periods. Many children will outgrow it, but some continue to have it into adulthood.
Does it need treatment?
Ongoing skin care and treatment will help control symptoms. Treatments focus on moisturizing the skin, avoiding irritant triggers and reducing inflammation. Good skin care can help prevent flare-ups:
- Moisturize skin regularly with thick creams or ointments (apply right after bathing)
- Use gentle, fragrance-free soaps and detergents
- Give lukewarm (not hot) baths
- Avoid known triggers like certain fabrics, soaps or foods
- Keep fingernails short to prevent scratching damage
- Use prescribed medications as directed by your doctor
When to see your child’s provider or a specialist?
- If the rash isn't responding to home care
- If you see signs of infection (oozing, crusting, fever)
- If the itching is severe and affects sleep or daily activities
- For help creating a treatment plan or adjusting medications
Interesting fact: Eczema is incredibly common, affecting up to 20% of children worldwide. About 60% of children who develop eczema will have their first symptoms before their first birthday, and most cases appear by age two.
Molluscum Contagiosum
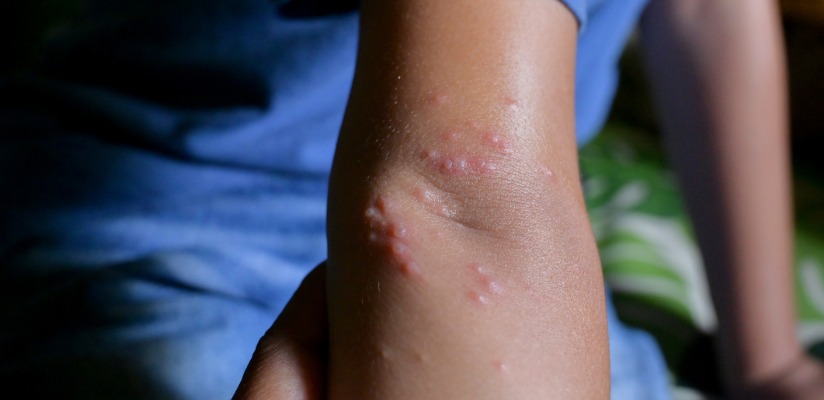
A virus called molluscipoxvirus causes molluscum bumps. It spreads through direct skin contact or sharing towels, clothing or bath items. It’s harmless but can be bothersome or unsightly. It usually goes away on its own but may take months to years to clear.
It’s highly contagious and can spread to other parts of the body or to other people.
Does it need treatment?
Treatment for molluscum isn’t necessary since it resolves on its own. Treatment may be recommended for cosmetic reasons, to prevent spread or if lesions are bothersome.
- Avoid scratching or picking at the bumps
- Don't share towels, clothing or bath items
- Cover lesions when possible, to prevent spread
- Keep skin clean and moisturized
Will it come back?
The virus can recur, especially if your child is re-exposed. Once all lesions clear, recurrence is less common.
When to see your provider or a specialist?
- If lesions are spreading rapidly or becoming numerous
- If lesions are on the face or genitals
- If you want to discuss treatment options
- If lesions become red, painful or infected
Interesting fact: While molluscum is often called "self-limiting," it can stick around much longer than most parents expect. The average time for molluscum to completely clear on its own is more than 13 months, and about 13% of children still have bumps after two years. Additionally, 41% of children spread it to siblings in the same household.
Impetigo
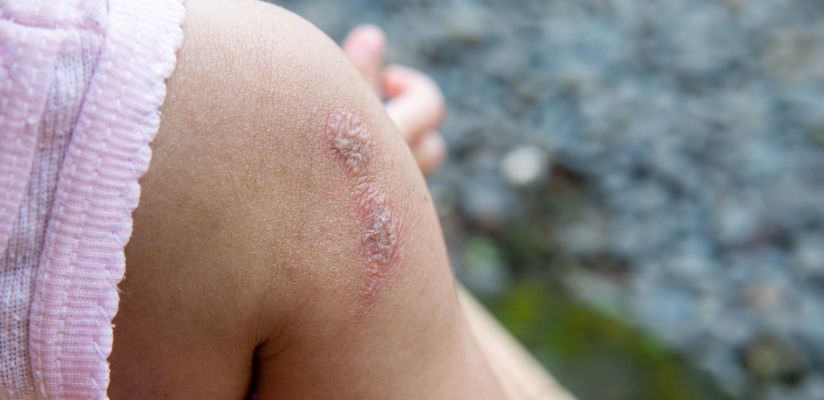
Impetigo is a bacterial infection caused by Staphylococcus aureus or Streptococcus (strep) bacteria. It often starts in areas where the skin is broken (cuts, insect bites, eczema).
It can spread quickly but usually is not serious if treated promptly. Impetigo is contagious and spreads through direct contact or sharing items like towels.
Good hygiene helps prevent recurrence but the rash can come back if your child is re-exposed to the bacteria.
Does it need treatment?
Treatment helps prevent the spread of Impetigo. An oral or topical antibiotic treatment helps it heal faster. To treat the rash at home:
- Keep the area clean and gently wash with soap and water
- Apply antibiotic ointment as prescribed
- Cover sores with gauze or bandages
- Wash hands frequently
- Don't share towels, clothing or bedding
- Keep your child's fingernails short and clean
When to see your provider or a specialist?
- As soon as you suspect impetigo, it needs antibiotic treatment
- If the infection is spreading despite treatment
- If your child develops a fever
- If sores don't improve after 2-3 days of treatment
Interesting fact: Impetigo is the third most common skin condition in children worldwide and affects more than 162 million children globally at any given time. It's most common in children aged two to five years old, and in the United States alone, there are more than 3 million cases every year.
Hives (Urticaria)
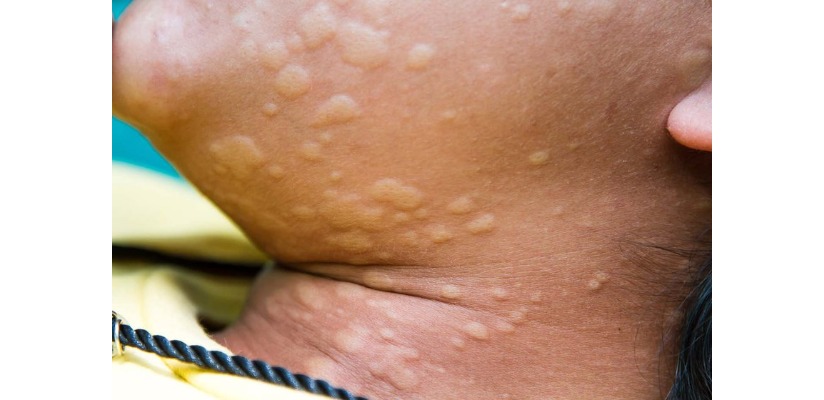
Hives are caused by a release of histamine in the skin. There are many possible triggers, but the most common are infections, foods, medications, insect stings or sometimes no clear cause. Hives are usually harmless and clean on their own.
Hives are not contagious. If the hives were caused by an infection, the infection itself may be contagious, but not the hives. Acute hives usually don't come back unless your child is exposed to the same trigger. Some children develop chronic hives that last longer than six weeks.
Does it need treatment?
Mild hives often don't need treatment. Antihistamines can help relieve itching and make hives go away faster. Here’s what you can do to provide relief at home:
- Give an antihistamine like diphenhydramine (Benadryl) or cetirizine (Zyrtec) for itching.
- Avoid giving topical antihistamines that are used directly on the skin.
- Apply cool compresses to itchy areas
- Avoid known triggers if identified
- Dress your child in loose, comfortable clothing
When to see your provider or a specialist?
- Call 911 immediately if your child has trouble breathing, face swelling or the rash spreads very quickly
- If hives last more than a few days
- If hives keep coming back
- If your child seems very uncomfortable despite home treatment
Interesting fact: Parents often blame food for their child's hives, but infections are actually the most common cause in children. Studies show that 51% of childhood hives are caused by viral or bacterial infections, while only about 3-9% are caused by food. In fact, in most cases (about 74%), no clear trigger can be identified at all.
Ringworm
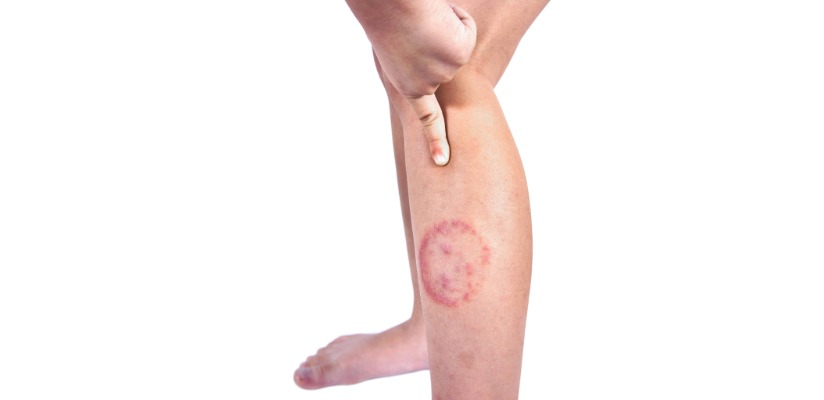
Ringworm can form on the scalp (Tinea Capitis) or on the body (Tinea Corporis). Both are caused by fungal infection caused by dermatophyte fungi. It spreads through direct contact with infected people, animals or contaminated surfaces.
Ringworm is contagious and can spread easily among children. Good hygiene and avoiding sharing personal items will help prevent recurrence.
Does it need treatment?
Treatment is needed to prevent the spread and possible hair loss if it’s on the scalp. If ringworm is on the body, most over-the-counter medications or prescribed antifungal creams will work.
If it’s on the scalp, oral antifungal medication should be taken for several weeks. Topical creams alone don’t work for scalp ringworm.
To provide relief at home:
Scalp:
- Give prescribed oral medication as directed (usually for 4-8 weeks)
- Use antifungal shampoo if recommended by your doctor
- Don't share combs, brushes, hats, or pillows
- Wash bedding and clothing in hot water
- Check other family members for signs of infection
Body:
- Apply antifungal cream as directed (usually for 2-4 weeks, even after the rash looks better)
- Keep the affected area clean and dry
- Wash hands after touching the rash
- Don't share clothing, towels, or sports equipment
- Wash clothing and bedding in hot water
- Check pets for signs of ringworm (hair loss, scaly patches)
When to see your provider or a specialist?
Scalp:
- As soon as you notice scaly patches or hair loss on the scalp
- If the condition doesn't improve after two weeks of treatment
- If you see signs of severe inflammation or pus-filled areas
- If hair loss is getting worse
Body:
- If the rash doesn't improve after two weeks of over-the-counter antifungal treatment
- If the rash is spreading or getting worse
- If your child develops multiple patches
- If the rash is on the face or widespread on the body
Interesting fact: Despite its name, ringworm has nothing to do with worms. It's actually a fungal infection. The name comes from the ring-shaped rash it causes on the body. Scalp ringworm is particularly tricky because it's the only type that requires oral medication—creams and ointments can't penetrate deep enough into the hair follicles to cure it.
Want to learn more about Dermatology at Le Bonheur?
DermatologyWant to find an appointment for your child?
Call 1-866-870-5570.





