Tech and Neuroscience: How technology is changing care for epilepsy and brain tumors
Posted: January 19, 2024Technology has changed our society and continues to create an impact on how we move through our days. Think about massive shifts in things like smartphones, artificial intelligence and robotic surgeries in just the past decade. It’s an impressive evolution.
In neuroscience, technology plays a key role—so much so that it has its own term: neurotechnology. James Wheless, MD, epileptologist, Le Bonheur Neuroscience Institute co-director, and chief of Pediatric Neurology, and Nir Shimony, MD, board-certified neurosurgeon with Le Bonheur Children’s Hospital, share what types of technology are used today and why they are so impactful in how they care for children with neurological conditions.
Crystal Clear Imaging
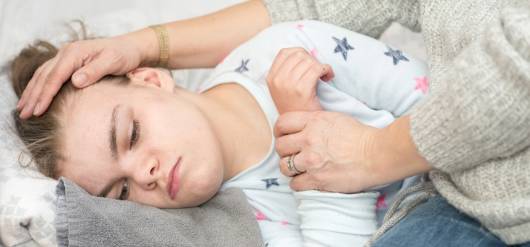
One application of neurotechnology is the ability to have a clear pictures of a child’s brain and where key functions live. This can help neurologists determine where an issue might be coming from, so that they can find the best way to address it. Technology also allows for neurosurgeons to not only look at the structure of the brain but also measure processes in the brain in real time. For example, this technology means they can see where speech or movement is coming from in the brain in a non-invasive and painless manner. This is especially important for planning neurosurgeries so that children have a surgery that fixes the original issue while avoiding key structures for speech and movement.
“Our improved ability to image the brain and target areas down to a very small scale has allowed us to treat children that in the past we couldn't treat. Our ability to assess brain function more accurately has allowed us to really hone in on the exact specifics of that prior to anything being done surgically,” states Wheless. “When our surgical colleagues have a discussion with the family, they can have a calm discussion well before surgery about the approach, how far away they are from critical areas of brain function and what to expect in the outcome. It's very different conversation from the years gone by.”
Cutting-Edge Technologies
Le Bonheur has always been at the forefront of incorporating new technologies especially in the realm of neuroscience. Because of that, Le Bonheur's Neuroscience Institute is one of the most advanced, from a technology standpoint, of any children's hospital in the world.
“We have all the current state-of-the-art imaging technology in one hospital that you can find anywhere in the world. It's really allowed us to take care of all sorts of children's problems, some of which in the past we just couldn't take care of,” shares Wheless.
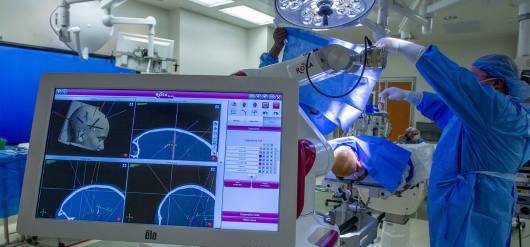
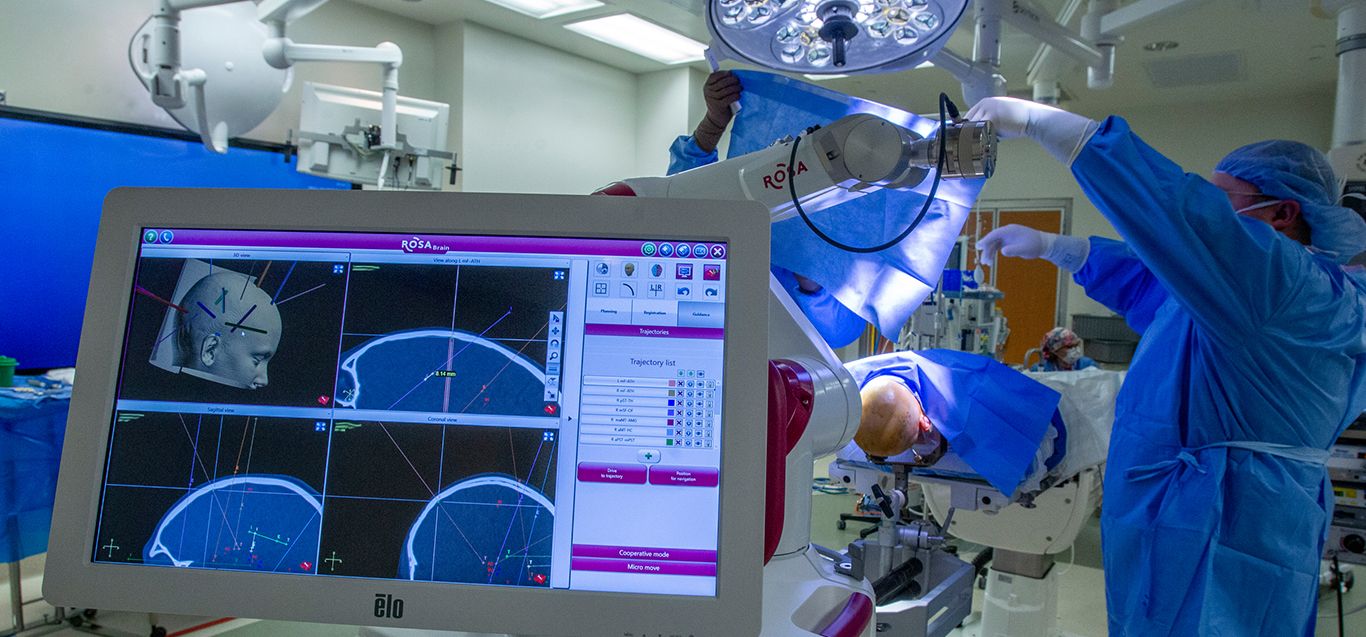
One of those technologies that has been added in recent years is the ROSA One Brain – a robot that provides precise guidance for instruments and brain mapping before surgery. Specifically, ROSA technology allows neurosurgeons access in the brain in the most accurate and minimally-invasive way possible. For example, electrodes that help neurosurgeons identify where seizures are in the brain.
“We get information from the brain itself regarding where the seizures are coming from. Where the network is that is affecting the epilepsy. And then of course, it helps us to have a much better way to treat the patients,” explains Shimony. “The incisions we make in order to implant those electrodes in the brain, are extremely small. We're talking about anything between 1-2 millimeters, where in the past we were talking about big surgeries. It's a completely different era.”
Another technology is iMRI, which stands for intraoperative MRI. Shimony describes this as a “magnificent” technology that optimizes both epilepsy treatment and tumor resection. It allows neurosurgeons to understand how well a procedure went and if any further surgery needs to be done while still in the operating room. Previously, patients would have to have an MRI after surgery and then return to the operating room if further surgery was needed.
“In epilepsy, this scan may reveal we need to disconnect more fibers, or if there is a tumor, we know if there is something left behind we need to take out. This completely changes the way we do surgeries,” he notes. “Because in our hospital, if we're taking tumors out, if we can, we're always going to get a gross total resection of the tumor. We are not okay with 95% resection, and the IMRI allows us to do it.”
These represent just two of the many neurotechnology options offered at Le Bonheur. Going forward, the neuroscience team welcomes new advancements to further improve patient outcomes.
The People Factor in Neurotechnology
One crucial component is required for these technologies to be successful and useful: experience individuals who use and operate the technology. Shimony and Wheless agree they are lucky to have a team with deep experience in neurotechnology applications. This becomes a key reassurance for referring physicians and patients alike.
“From my standpoint, the biggest advantage with all the technology is for referring physicians. It really makes it easy for them because it's kind of one-stop shopping. Based on the patient and their individual needs, we will determine which testing is best. And, we have it all available so they don't have to think about anything,” shares Wheless.
“Whoever wants to come, either families or referring physicians, we want them to know we have the technology but also a large staff with a lot of experience in the field of epilepsy and oncology,” adds Shimony. “This allows us to give a different kind of experience to the families, to the patients, and eventually, what's more important, the results themselves.”
Want to learn more about Clinical Neurosciences at Le Bonheur?
Clinical NeurosciencesWant to find an appointment for your child?
Call 1-866-870-5570.