Le Bonheur's comprehensive epilepsy program provides advanced treatment options for your child's seizures. Responsive neurostimulation (RNS) is a device that is placed in a patient’s skull by a pediatric neurosurgeon as an epilepsy surgery treatment option. The device is connected with electrodes to the part of the brain responsible for seizure activity. The location of these electrodes is based on evaluation in the Epilepsy Monitoring Unit (EMU) and is individualized for each patient.
The device is programmed by a pediatric neurologist to detect pre-seizure brain activity and disrupt any abnormal brain seizure activity with electrical impulses to prevent seizures.
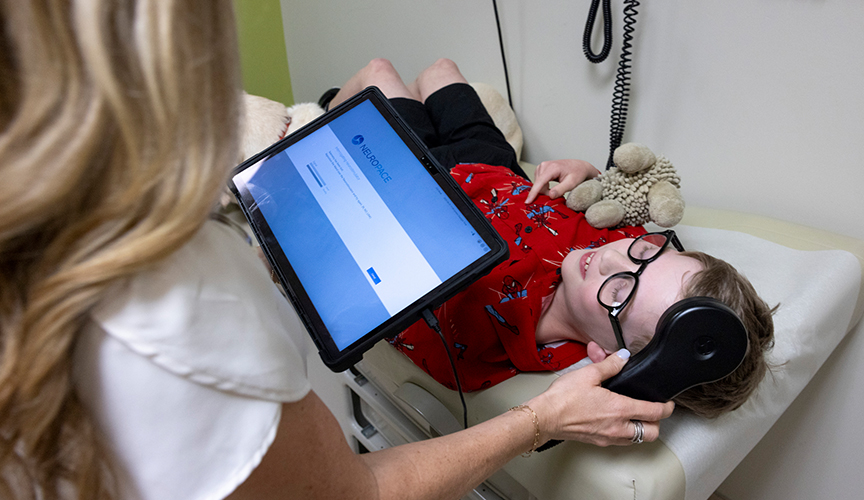
How does responsive neurostimulation (RNS) work?
- RNS is implanted in the skull with electrodes connected to the area of the brain responsible for seizure activity.
- The RNS device continuously watches the brain's electrical activity for anything out of the ordinary.
- When the device detects abnormal electrical activity, it responds by delivering a small dose of electrical stimulation to normalize the abnormal activity before the individual experiences a seizure. The electrical stimulation is imperceptible -- the person with the implanted device cannot feel it.

Who is eligible for responsive neurostimulation (RNS)?
- Responsive neurostimulation (RNS) is approved for young adults ages 18 and older and on a limited basis in children primarily 10 years or older.
- Responsive neurostimulation (RNS) device implantation can be an epilepsy surgery option for those who have not had success controlling seizures through medication.
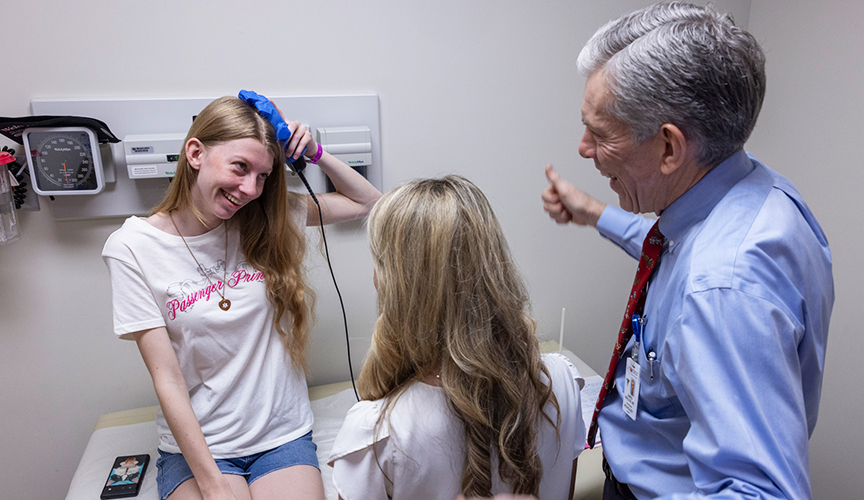
Facebook Live
Le Bonheur patient Hannah Lawrence sits down with Neuroscience Institute Co-Director James Wheless, MD, to talk about about responsive neurostimulation (RNS) devices and her experience with epilepsy surgery.




