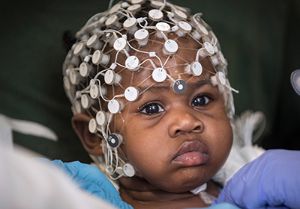
Mended Hearts
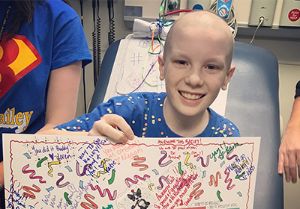
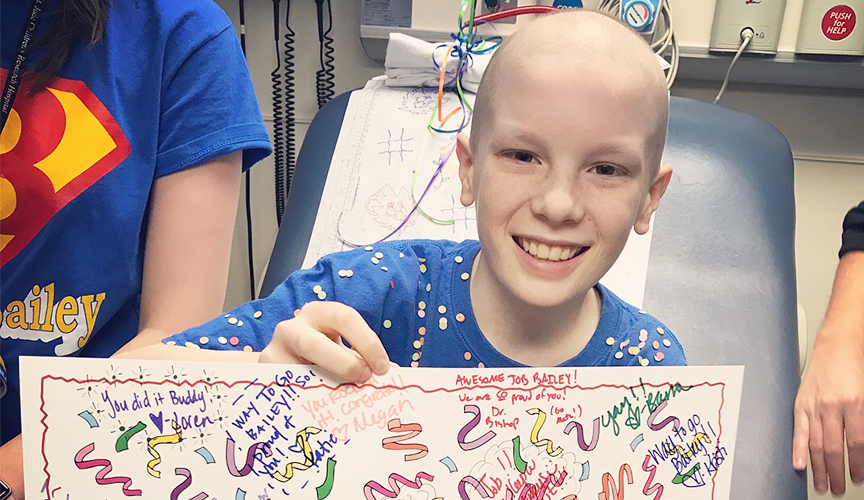
Middle school cross-country runner Bailey Jessop had complained of leg pain for weeks.
His mom, Le Bonheur physical therapist Kimberly Jessop, hoped it was growing pains. But Bailey had just signed up for a road race series with his dad, and Kimberly’s gut told her to get it checked out just in case.
The verdict: osteosarcoma that required 40 weeks of aggressive chemotherapy, several surgeries to remove part of his femur and a new titanium prosthesis.

“The chemotherapy was so harsh on his body. He had an ECHO before every treatment,” Kimberly said. “Toward the end of the treatment, we started to see signs of cardiomyopathy.”
The chemotherapy that attacked Bailey’s cancer eventually weakened his heart — presenting a new battle for Bailey. It’s a reality that was not surprising to the Jessops, considering how cancer and its treatments can affect multiple systems.
It’s also a reality that cardiologists at Le Bonheur Children’s Hospital are working to change.
Today, more than 80% of children who are diagnosed with cancer will survive, thanks to advancements in cancer care. But that doesn’t mean they all escape unscathed.
Long-term cardiovascular complications are now the leading cause of non-cancer morbidity and mortality in long-term childhood cancer survivors.
The growing population of childhood cancer survivors led Le Bonheur’s Heart Institute to establish a formal cardio-oncology clinic at St. Jude Children’s Research Hospital to care for those children. The challenge for them is clear: improve the quality of life for kids like Bailey and work to ensure that children with cancer don’t also have to worry about weakened hearts.
Le Bonheur Heart Institute cardiologists specialize in chemotherapy-induced cardiovascular toxicity (including cardiomyopathy) in order to treat childhood cancer patients and survivors who now have weakened hearts.
New Knowledge Is Needed
Chemotherapy-induced cardiovascular toxicity is an emerging problem for pediatric cardiologists, as a new population of patients fight off the cancer that would have killed them more than a decade ago. Today, St. Jude estimates that there are more than 420,000 childhood cancer survivors in America.
Within Le Bonheur’s cardio-oncology program, cardiologists provide heart care to St. Jude patients receiving treatment, as well as survivors who are experiencing late effects of cancer treatment.
.png?language_id=1)
Jeffrey A. Towbin, MD, serves as chief of Cardiology at both Le Bonheur and St. Jude and established the clinical and research facets of the program after he was recruited to Memphis five years ago. Under his leadership, Le Bonheur has since recruited four cardiologists to focus on chemotherapy-induced cardiovascular toxicity.
“The field must train cardiologists with expertise in cardio-oncology,” said Towbin, who also serves as executive co-director of Le Bonheur’s Heart Institute and St. Jude Chair of Excellence in Pediatric Cardiology. “We are seeing large numbers of patients who have received cancer chemotherapy and may have developed cardiovascular abnormalities or will develop cardiovascular dysfunction in the future.”
Towbin says he believes more research is needed to understand the basic mechanisms that cause certain children to be at higher risk than others — and that research would facilitate the development of preventative measures, as well as targeted treatment for affected individuals.
For example, literature suggests that the anthracyclines class of cancer drugs can cause dilated cardiomyopathy, where the heart becomes enlarged and squeezes poorly. In Memphis, though, cardiologists have found that, in addition to dilated cardiomyopathy, many children at St. Jude develop a problem with heart relaxation, called restrictive cardiomyopathy or restrictive physiology. Therapies are different between dilated and restrictive cardiomyopathy.
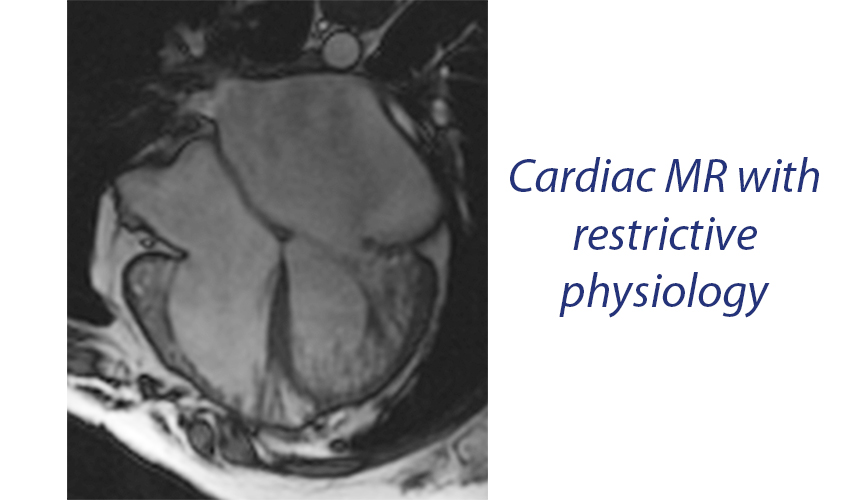
“In addition, newer agents being used now have significant potential for affecting cardiovascular function and, in fact, may have even more significant impact. New knowledge is needed,” Towbin said.
Pediatric Cardiologist Jason Goldberg, MD, was recruited to Memphis after his fellowship at Texas Children’s Hospital — a heart failure and transplant center where he saw an increasingly high number of children and young adults who had developed heart failure after undergoing cancer therapy.
“Specialists at St. Jude had similarly found accelerated rates of heart attacks and cardiac death among young adults who had received chemotherapy,” Goldberg said. “While specific chemotherapies, such as high-dose anthracyclines, have known cardiotoxic profiles, I observed significant cardiomyopathy and heart failure among children who had not received high doses of anthracyclines.”

Additionally, many children who have undergone chemotherapy have heart rates and blood pressures that are higher than normal, Goldberg said.
“I believe that identifying and treating these early subtle signs of heart disease in children undergoing cancer therapy can prevent future heart disease and heart failure,” he said. “This work is most salient at St. Jude, where more children have had successful cancer treatment than anywhere else.”
Goldberg believes the collaboration with St. Jude, Le Bonheur and the University of Tennessee Health Science Center (UTHSC) will allow his team to better treat heart disease among survivors and comprehensively examine the long-term cardiovascular effects of cancer therapy.
“Children suffering from cancer shouldn’t have to also worry about their hearts,” said Pediatric Cardiologist Gary Beasley, MD. “We have an opportunity to work together between oncology and cardiology to develop strategies to treat cancer while minimizing the cardiovascular effects. It’s an emerging field where two complex disciplines cross.”
Finding Answers
The Le Bonheur Heart team — along with their colleagues at St. Jude — launched four active studies and have others awaiting IRB approval. The studies consider anthracycline-induced cardiotoxicity and other trends they’ve noticed in their patients.
One of those studies, “Acute Hemodynamic Effects of Pediatric Hematopoietic Cell Transplantation,” examines the cardiovascular risks of childhood hematopoietic cell transplantation — particularly less-studied conditions like hypertension, tachycardia and cardiac dysfunction. After finding a high prevalence of these conditions in a study group of 150 transplantation patients, the group presented initial work at the 2019 American Society of Bone Marrow Transplantation Meeting. Le Bonheur scientists are working alongside UTHSC and St. Jude researchers in this work.
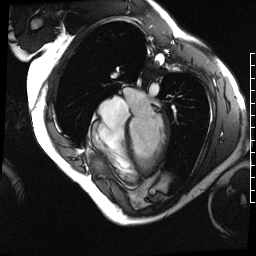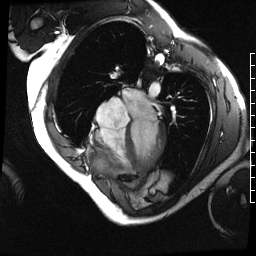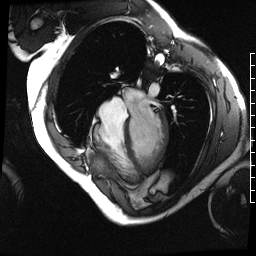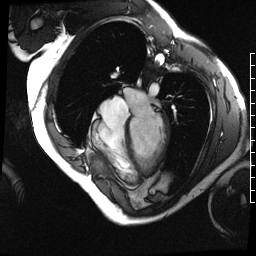
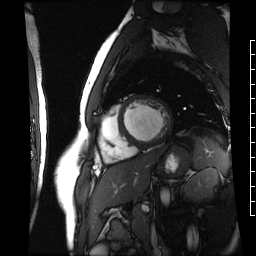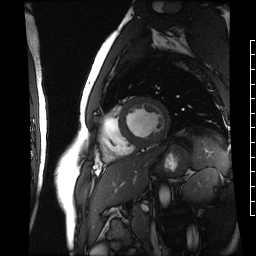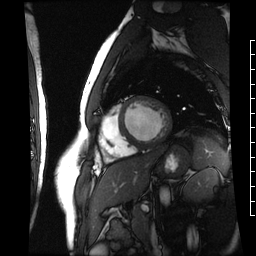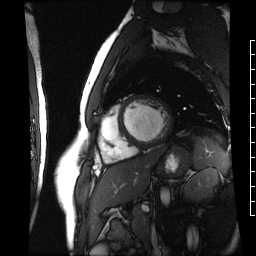
Chemotherapy-induced cardiomyopathy will decrease function and cause a dilated ventricle. Above is a four-chamber cardiac MRI, and below is a short-axis cardiac MRI from a patient with chemotherapy-induced cardiomyopathy.
Teams of Le Bonheur and St. Jude investigators have started to present very early work to groups studying pediatric hematology and transplantation and cellular therapies.
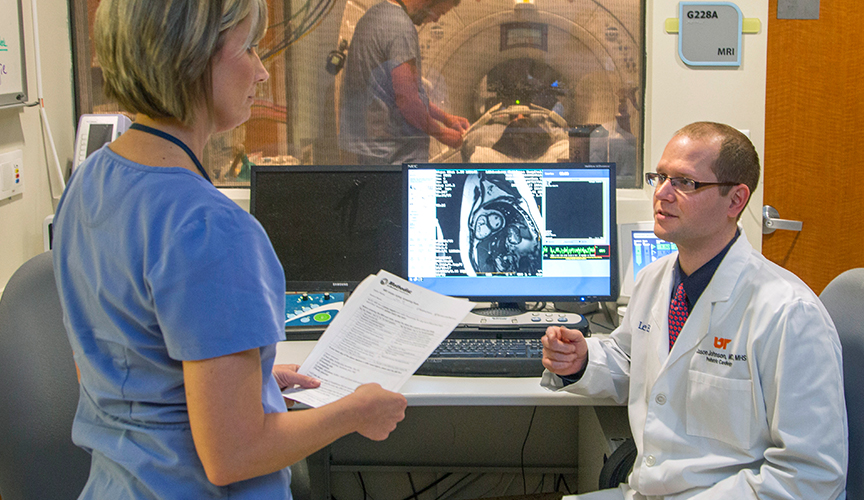
Meanwhile, Pediatric Cardiologist and Cardiac MRI Director Jason Johnson, MD, knows from his work that some children’s hearts can tolerate chemotherapy much better than others. He’s working with cardiac MRI mapping to better understand each heart’s tissue characterization – and hopefully develop prediction models for future cardiomyopathy.
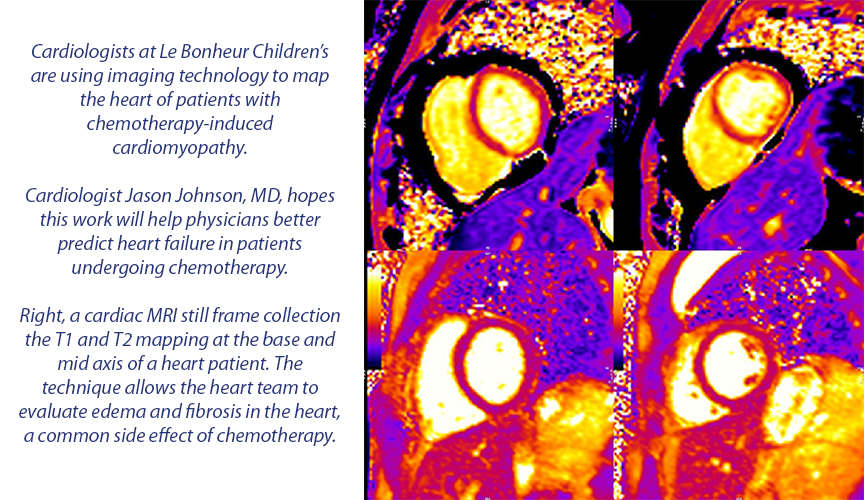
“We don’t know why some children suffer heart failure after chemotherapy, but we think mapping can help us predict,” Johnson said. “That understanding will lead to better therapies for chemotherapy-induced cardiotoxicity.”
Bailey’s mom, Kimberly Jessop, is betting on the entire Le Bonheur team and hopes that research will develop better outcomes. She knows that Bailey still has a long road ahead, even if the cancer is gone. But she says that she’s grateful to be near a team of doctors willing to research how cancer drugs change the heart and prevent side effects when they are preventable.
“For us, that means a better quality of life for our son and so many others like him,” she said. “I wasn’t confident that Bailey’s heart damage was correctable, but I was confident we were in the best place.”
Cardio-Oncology Research
- Systolic dysfunction and chemotherapy
- Systolic dysfunction and radiotherapy
- Stress-induced cardiomyopathy
- Cardiovascular biomarkers in patients with cancer
- Diastology in the patient with cancer and hematologic diseases
- Cardiovascular noninvasive imaging in the oncology patient
- Electrophysiology anomalies
- Pericardial disease
- Pulmonary hypertension
- Thromboembolism
- Systemic hypertension
- Cardiac masses
- Primary and secondary prevention of cardiovascular toxicity
- Congenital heart disease in the oncology patient
- Peri-operative evaluation and management of the cardio-oncology patient
- Cardiothoracic surgery in children with cancer
- Genetics of cancer and cardiac toxicity
- Genetic pathways of cancer and cardiac disease
- QOL in children and young adults with cancer
- Invasive/interventional cardiology in patients with cancer
- Systolic dysfunction and chemotherapy
Help us provide the best care for kids.
Le Bonheur Children's Hospital depends on the generosity of friends like you to help us serve 250,000 children each year, regardless of their family’s ability to pay. Every gift helps us improve the lives of children.
Donate Now