Orthopedics
Comparing Imaging Modalities for Spinal Compression Fractures
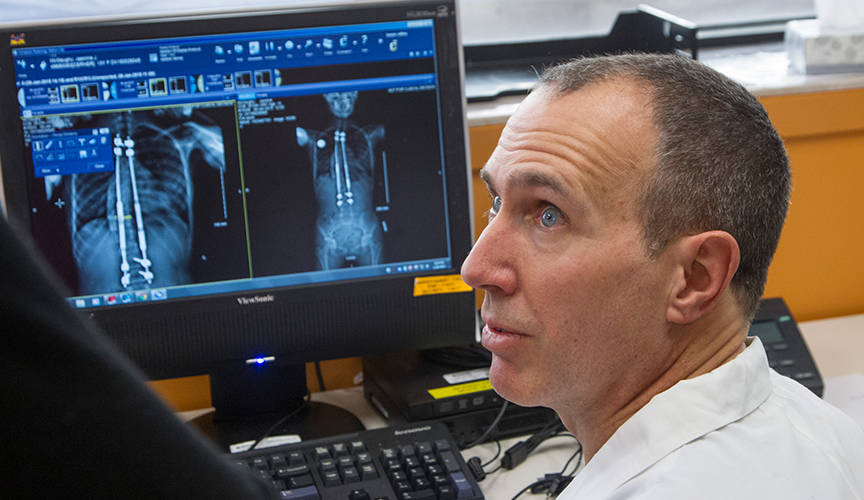
In adolescents and children, thoracic and lumbar compression fractures are among the most commonly observed spinal fractures. Compression fractures occur when vertebrae collapse due to trauma or conditions such as osteoporosis. Compression fractures are usually detected by computed tomography (CT) because it provides a complete picture of cranial, thoracic and abdominal injuries. However, some centers use magnetic resonance imaging (MRI) instead of CT because it does not involve the use of ionizing radiation. Moreover, unlike CT, MRI can show soft tissue damage in addition to vertebral fractures. However, MRI is more costly than CT, and young children often require sedation for MRI, further exacerbating the cost.
Given the use of both CT and MRI in diagnosing compression fractures, Orthopedist Jeffrey R. Sawyer, MD, and colleagues sought to compare the sensitivity of these imaging modalities in diagnosing thoracic and lumbar compression fractures. They examined data from 52 patients with thoracic or lumbar fractures who underwent both CT and MRI scans at Le Bonheur. A total of 191 fractures were identified with an average of 3.7 fractures per patient. MRI and CT showed complete agreement in 44% of patients, with CT missing fractures in only 2% of patients. Since the overall sensitivity of CT was 98% and MRI did not detect additional tissue injury, the investigators suggested the use of CT alone is sufficient to diagnose thoracic and lumbar compression fractures.
Hemoglobin and Disease Severity in Early Onset Scoliosis
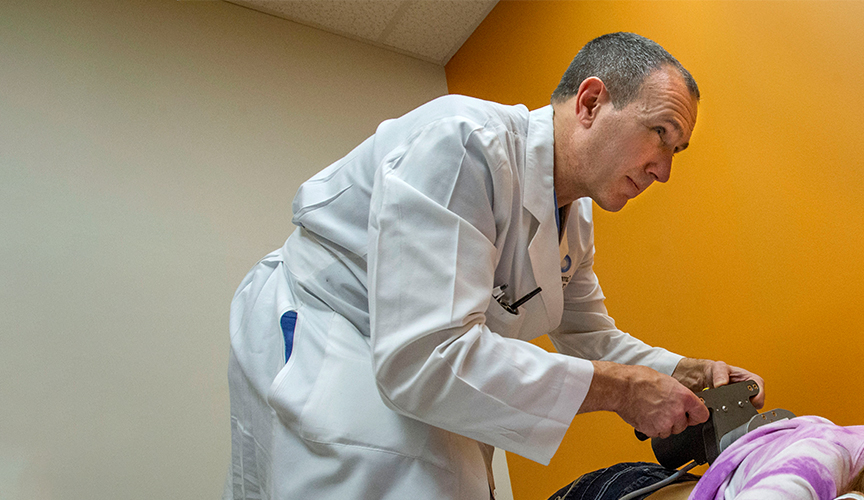
In early onset scoliosis, the abnormal curvature of the spine reduces the available space in the chest cavity, effectively restricting the expansion of the lungs and decreasing pulmonary function. In severe cases, early onset scoliosis results in thoracic insufficiency syndrome, a dangerous condition in which normal breathing and lung growth are restricted. The pulmonary function test is currently considered the best tool for assessing the severity of this disease. However, the pulmonary function test is difficult to perform in children, leaving physicians to rely upon radiographic measures that do not accurately reflect disease severity.
Orthopedist Jeffrey R. Sawyer, MD, and collaborators at other children’s hospitals decided to examine another potential marker of disease severity: elevated hemoglobin. Elevated hemoglobin correlates with hypoxia and may also reflect the severity of early onset scoliosis prior to surgery. Measuring hemoglobin in children is also easier than pulmonary function testing because it only requires a blood draw. To examine the relationship between the severity of pre-operative early onset scoliosis and hemoglobin levels, the investigators measured hemoglobin prior to corrective surgery and at 6, 12 or 18 months post-surgery in 268 patients. They also measured the degree of spine curvature before and after surgery.
Sawyer and colleagues identified 48 patients who had elevated hemoglobin levels prior to surgery. The patients with elevated hemoglobin were younger than those with normal hemoglobin, but no other marked differences between the groups emerged pre-operatively. Following surgery, hemoglobin was measured in 27 of the 48 patients with elevated hemoglobin. These measurements revealed a significant reduction in postoperative hemoglobin at 6 months and an overall reduction at 18 months. Patients without elevated hemoglobin before surgery showed no changes in hemoglobin after surgery.
The investigators concluded elevated hemoglobin could potentially serve as a marker of disease severity. However, elevated hemoglobin appeared in only a subset of patients, indicating it may be useful in only the most severe cases. Ultimately, the investigators concluded that the best approach for evaluating early onset scoliosis may be a battery of assessments, such as radiographic measurements, hemoglobin levels and patient feedback.
Help us provide the best care for kids.
Le Bonheur Children's Hospital depends on the generosity of friends like you to help us serve 250,000 children each year, regardless of their family’s ability to pay. Every gift helps us improve the lives of children.
Donate Now